Antibiotics are often the default treatment path for many doctors when it comes to Lyme disease. However, they are not always effective. Lyme disease is a complicated disorder that we don’t yet fully understand. Yes, antibiotics work to a certain degree, but in some cases they don’t fully eradicate the disease, leading to years of debilitating symptoms for patients. So when are antibiotics effective, which types are effective, and in cases where they fail to get rid of the Lyme bacteria, what happens? These aren’t easy questions to answer, as much Lyme disease knowledge is still murky at best. However, it’s important to try to understand exactly how antibiotics and Lyme disease work in tandem.
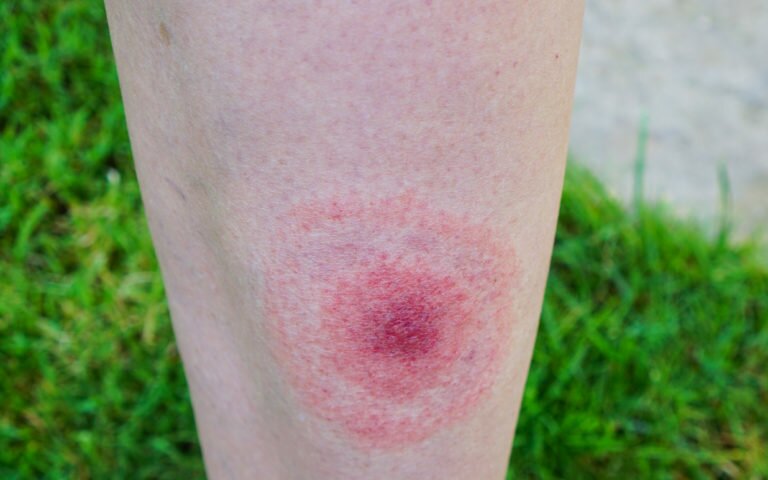
Firstly, let’s look at when they are effective. Lyme disease can be broadly split into two stages: acute and chronic. Acute Lyme lasts for a few weeks, and is easily identifiable by the presence of a bullseye rash. This distinctive Lyme symptom is present in the majority of cases in the initial stages of the disease, and is one of the best indicators available to doctors and patients alike. If the condition is presented to a medical professional in the acute stages, Lyme disease can almost always be eradicated by antibiotics. Successful treatment is usually achieved by a short course of oral antibiotics, namely doxycycline or amoxicillin. However, if this acute stage of the disease is missed and it progresses to the chronic stage, antibiotics alone will not be enough to fight off the disorder.

Chronic Lyme disease is a much more diverse and complicated condition than acute Lyme. This is because inflammation also plays a significant role in the symptoms. Many doctors follow the traditional line of thinking that Lyme, being caused by the presence of bacteria, can be treated successfully using synthetic microbes (i.e. antibiotics), like many other conditions and diseases. While this reasoning may be structurally sound, it doesn’t take into account the body’s own reaction to the bacteria, and how that can kickstart a whole set of new and debilitating symptoms. On top of that, individuals will have different reactions to the borrelia bacteria, depending on their constitution. Lyme disease is not a one-size-fits-all condition like the flu, which has very little variance in its symptoms on a person-to-person level.
The symptoms of chronic Lyme vary wildly, but usually include joint pain, muscle pain, aches, soreness and a chronic sense of fatigue. All these symptoms are a result of the immune system’s response to the bacteria. For some reason, the immune system goes into overdrive when faced with a long-term borrelia infection, resulting in severely debilitating symptoms, even when the actual presence of the bacteria may be minimal. Obviously, antibiotics administered at this point will have zero effect on inflammation symptoms, as they are the body’s own doing. Yet Lyme-illiterate doctors will often insist on antibiotics as the only treatment path for chronic Lyme disease, if they believe the diagnosis at all (chronic Lyme is still not officially recognised by the CDC).
Treating chronic Lyme requires a more nuanced touch. The medical staff at BCA-clinic in Augsburg, Germany, have been experts in Lyme disease for a long time. Their approach to treatment is designed to tackle both the inflammation and infection symptoms of the disease. The first thing to do is test the patient to see what the ratio of inflammation and infection actually is. Some people might have a lot of inflammation and only traces of a bacterial infection, while some others might have the complete opposite. Successful Lyme disease treatment constitutes knowing the difference between the two, and responding accordingly. Antibiotics are only half of the approach here, as they solely deal with infection. For the inflammatory symptoms, herbal supplements and diet adjustments are necessary.

Borrelia bacteria have been proven to be surprisingly resistant to antibiotic treatment. If they are left in the system, they can adapt to survive the natural immune response, as well as tolerating various forms of common antibiotic. Borrelia exists in two separate forms: the spirochete and the ‘cell wall’ variant, sometimes known as the ‘cyst’ form. Under stress, the spirochete will adapt to the cyst form, making it much more resistant to antibiotics. It is likely that the majority of chronic Lyme sufferers have both borrelia forms present in their systems at any given time. Therefore, it is crucial to combine antibiotics in order to attack the bacteria from all angles. This requires an experienced medical professional who is well-versed in Lyme; unfortunately, many doctors are not.
It’s important to back up any heavy antibiotic use with a probiotic, in order to keep your gut healthy. Knowing how long to stay on a course of a particular antibiotic is also necessary. If you suspect you have chronic Lyme disease, getting help from an expert in the field should be paramount. The disease can affect people for many years, and is very hard to treat if you don’t know what you’re doing. While antibiotics are an important component, they are not totally reliable in every case. When it comes to chronic Lyme, they should be used as part of a broader treatment process.